Telemedicine: How Digital Consultations Are Reshaping Healthcare
Telemedicine has moved from being a supplementary healthcare option to becoming a core component of modern medical practice. Through secure digital platforms, patients can now access qualified medical professionals regardless of geographical limitations. This transformation is redefining how care is delivered, managed, and experienced.
Driven by advancements in communication technology and changing patient expectations, telemedicine addresses long-standing challenges such as accessibility, continuity of care, and time efficiency. This article explores how telemedicine evolved, how it works in practice, and why it has become a trusted model within healthcare systems worldwide.
The Evolution of Remote Medical Care
Early forms of telemedicine emerged through telephone-based consultations and radio communication in remote regions. These early efforts aimed to bridge healthcare gaps where physical access to doctors was limited.
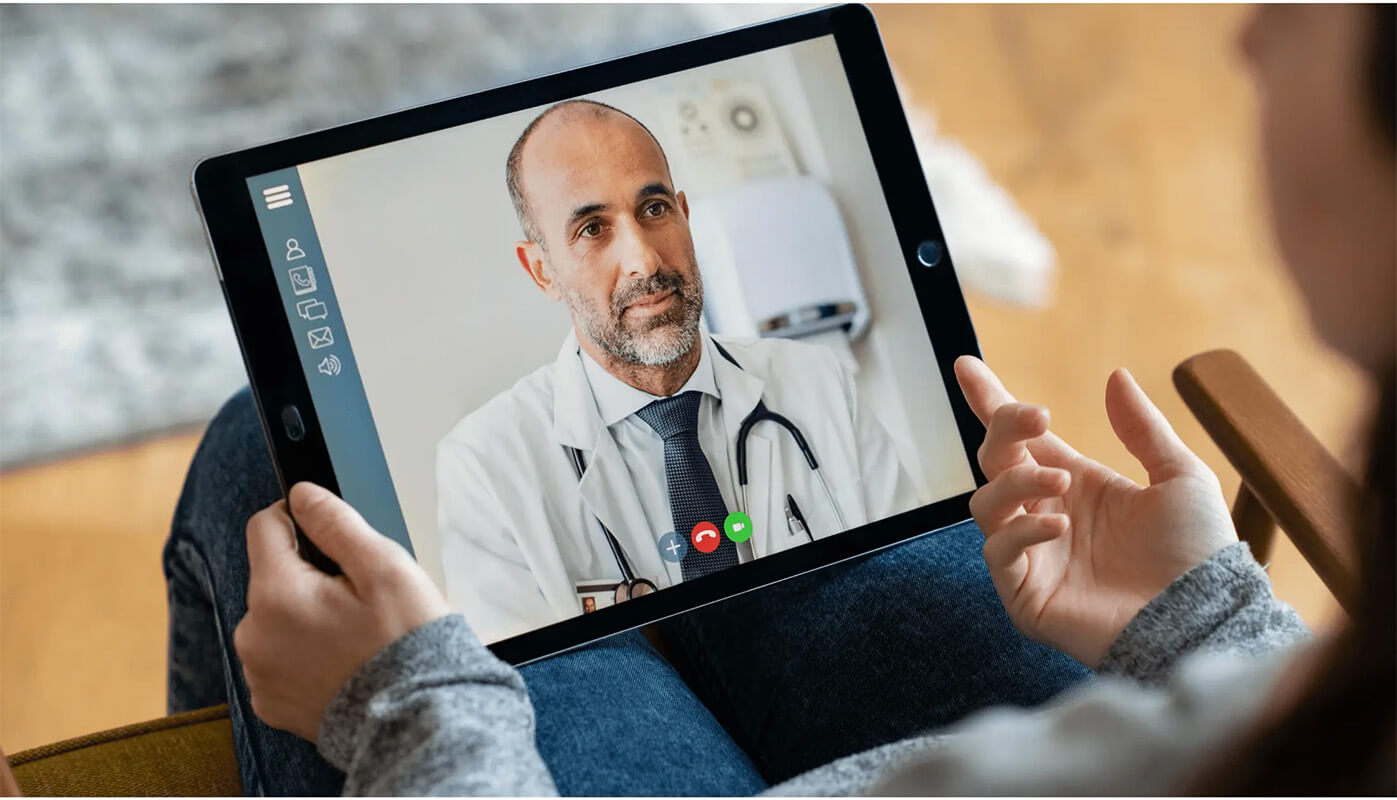
With the expansion of internet infrastructure, digital consultations evolved into secure video-based interactions, enabling doctors to visually assess patients, review records, and provide structured medical guidance.
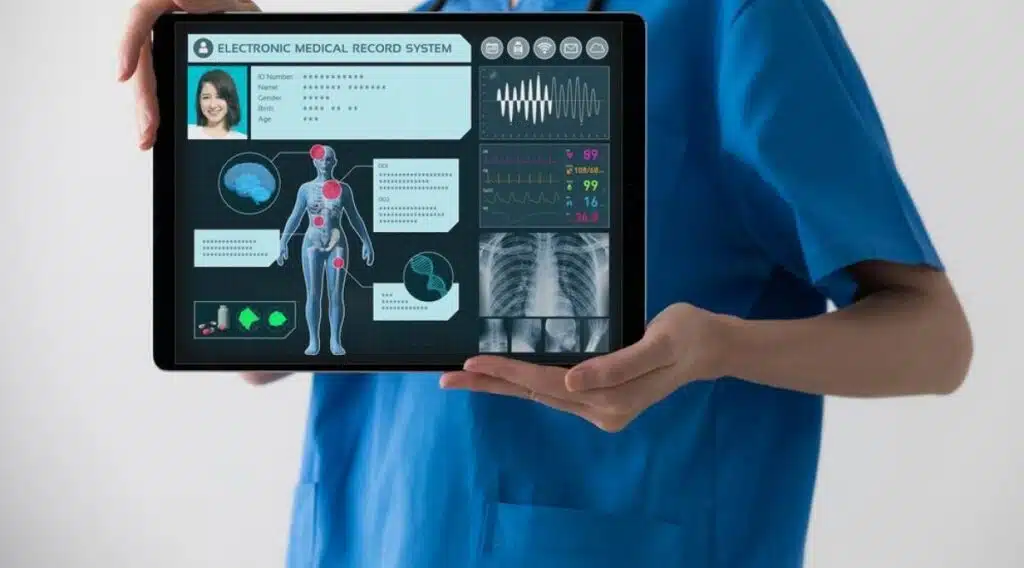
Today, telemedicine integrates electronic health records, diagnostic sharing, and follow-up tracking, making it a clinically reliable extension of traditional care.
Clinical Structure and Patient Safety
Contrary to common misconceptions, telemedicine consultations follow defined clinical protocols. Medical history intake, symptom evaluation, and risk assessment remain central to the process.
Licensed physicians apply evidence-based decision-making while clearly identifying cases that require in-person examination or emergency intervention. This structured approach ensures that patient safety remains the primary priority.
Secure data handling and confidentiality protocols further support ethical medical practice in virtual environments.
Improving Access and Continuity of Care
Telemedicine plays a critical role in improving healthcare access for individuals in rural or underserved regions. Patients who previously faced long travel times can now receive expert medical advice without leaving their communities.
For chronic disease management, telemedicine supports continuity of care through regular follow-ups, medication guidance, and monitoring of long-term conditions.
This ongoing connection helps reduce complications, hospital admissions, and treatment disruptions.

Ethical Responsibility and Medical Limitations
While telemedicine offers significant advantages, it is not intended to replace all forms of in-person care. Ethical practice requires transparency regarding its limitations.
Doctors must clearly communicate when physical examinations, imaging, or emergency care are necessary. Responsible telemedicine strengthens healthcare systems by working alongside traditional services, not replacing them.
Clear boundaries and professional accountability preserve trust between patients and medical providers.
The Future of Digital Healthcare
As technology continues to advance, telemedicine is expected to integrate artificial intelligence, remote monitoring devices, and predictive analytics to further enhance clinical decision-making.
However, human judgment, empathy, and ethical responsibility will remain central to medical practice. Telemedicine’s success lies in balancing technological efficiency with compassionate care.
Conclusion
Telemedicine represents a fundamental shift in how healthcare is delivered, offering accessibility, continuity, and professional medical guidance through digital means.
When implemented responsibly, it strengthens patient engagement and supports healthcare systems in meeting modern demands while preserving clinical integrity.



Leave a Reply